7 Warning Signs Your Dog Has Dental Disease (Don't Ignore #4)
More than 80 percent of dogs over age three have active dental disease — yet most of them show no obvious signs. They keep eating. They keep playing. They keep wagging their tails. Meanwhile, bacteria are destroying the bone that holds their teeth in place. These 7 warning signs are what your dog cannot tell you but their body reveals anyway. Read each one carefully — #4 is the one most owners dismiss until it is too late.
Why Dogs Hide Dental Pain — The Truth Vets Know
Before we go through the signs, you need to understand something that changes how you think about your dog's dental health entirely.
Dogs are descended from predators. In the wild, showing weakness — pain, illness, vulnerability — is a survival risk. An animal that limps is the one that gets left behind. An animal that stops eating is the one that starves. So over tens of thousands of years, dogs evolved a powerful biological drive to mask discomfort and carry on normally. This instinct does not switch off in domestic pets.
According to VCA Animal Hospitals, one of the largest veterinary networks in the United States, dental disease is one of the most common conditions seen in practice — and "few dogs show obvious signs of dental disease, so it is up to the dog's family and veterinarian to uncover this hidden and often painful condition." That phrase — hidden and often painful — is the most important thing in this article.

Your dog may be experiencing significant chronic oral pain right now, while still eating their dinner, fetching their ball, and jumping up to greet you. The seven signs below are what breaks through that masking instinct. They are the moments when the pain or the disease has progressed enough that the body cannot hide it anymore.
Critical point: The absence of obvious distress does not mean your dog is comfortable. If you see any of these seven signs — even just one — take it seriously. The disease has been present and progressing for weeks or months before any sign becomes visible.
Sign #1 — Persistent Bad Breath (Halitosis)
Persistent Bad Breath
Every dog has some degree of breath odour — mild, up-close unpleasantness that comes from being a carnivore. That is normal. What is not normal is breath that is consistently offensive at conversational distance, that persists throughout the day regardless of when your dog last ate, and that has that distinctive rotten or sulphurous quality.
Bad breath in dogs is caused by volatile sulphur compounds — molecules produced by anaerobic bacteria feeding on plaque, tartar, and dying gum tissue. These bacteria thrive in the oxygen-poor environment beneath the gum line. The smell is their metabolic waste. The stronger and more persistent the smell, the heavier the bacterial load — and the heavier the bacterial load, the more advanced the disease.

The common owner mistake here is normalising it. "All dogs have bad breath," owners say. Most vets cringe when they hear this. A healthy dog with clean teeth and healthy gums does not have breath that clears the room. If yours does, the bacteria are already at work.
How to check: Sit close to your dog when they are calm and breathing normally. If you can clearly smell their breath without putting your nose near their mouth, it is beyond normal. If the smell is consistently present — not just after they ate something unusual — it is almost certainly dental disease.
What to do: Begin daily brushing with enzymatic toothpaste immediately. Add a VOHC-approved dental chew daily. Add a tasteless water additive like Oxyfresh to the water bowl. If bad breath persists after 3 weeks of consistent home care, schedule a veterinary dental examination — you likely have tartar that needs professional removal.
Sign #2 — Visible Yellow or Brown Deposits on the Teeth
Tartar Buildup on Teeth
Healthy dog teeth are white to slightly cream-coloured. Any yellow, tan, or brown coating on the tooth surface — particularly concentrated along the gum line — is tartar (calculus). Tartar is mineralised plaque: the bacteria-laden film that forms on teeth within hours of eating, left undisturbed long enough to harden into a rock-like deposit.
This matters enormously for one reason: once tartar hardens, no amount of home care removes it. You cannot brush it off. Dental chews cannot dissolve it. Water additives cannot penetrate it. Only professional veterinary scaling under anaesthesia — the same process your dentist uses on your teeth, but requiring general anaesthesia in dogs — will remove established tartar.
The most common location to spot early tartar is the upper canine teeth (the long pointed teeth) and the large upper back molars, viewed from the cheek side. These surfaces are where the salivary glands deposit minerals fastest. Gently lift your dog's upper lip and look at these areas in good daylight. Yellow or brown buildup is visible to the naked eye long before it becomes a clinical emergency.
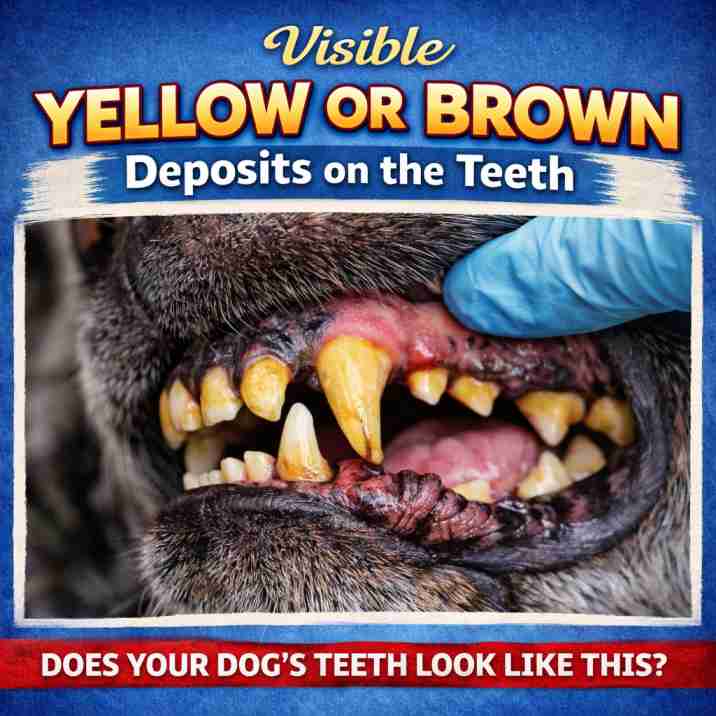
According to the Merck Veterinary Manual (2026): Back teeth are affected more often than front teeth. Upper teeth are affected more severely than lower teeth. The outer surfaces — cheek-facing side — have more disease than surfaces near the tongue. Check these spots specifically when examining your dog's mouth.
What to do: If visible tartar is present, schedule a veterinary dental cleaning. Begin daily brushing immediately to prevent new tartar from forming while you wait for the appointment. Tartar that is left in place causes the gum inflammation that progresses to bone loss — so the cleaning is not optional, it is necessary.
Sign #3 — Red, Swollen, or Bleeding Gums
Inflamed or Bleeding Gums (Gingivitis)
Healthy gums in a dog should be pale pink, firm to the touch, and smooth along the gum line where it meets the tooth. They should not bleed when you gently press them with a clean finger. Any deviation from this — redness, puffiness along the gum edge, dark red line at the tooth-gum junction, or bleeding when touched — is gingivitis: active bacterial inflammation.
Gingivitis is caused by bacterial toxins in tartar irritating the gum tissue. As the Colorado State University Veterinary Teaching Hospital explains, red gums are usually the first clinical sign of dental disease that owners can observe. It is the point where the disease has become visible — but crucially, it is also the last point at which the condition is fully reversible.
Remove the tartar through professional cleaning, eliminate the bacteria through consistent home care, and gum tissue can return to full health. Beyond gingivitis — once the disease progresses to periodontitis — the damage to ligaments and bone is permanent. No procedure restores lost bone. This makes gingivitis not just a warning sign but a genuine last-chance moment to intervene before irreversible harm occurs.
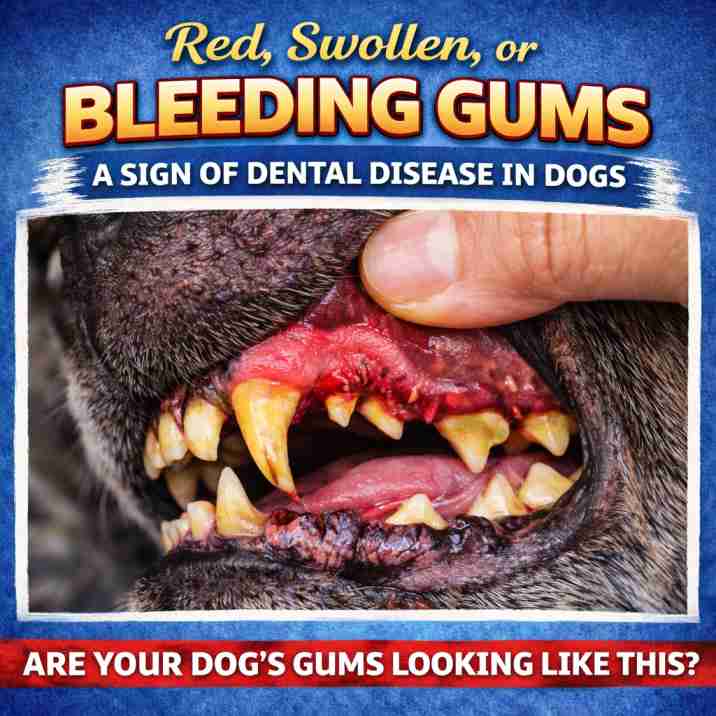
The 2-second gum check: Gently lift your dog's upper lip. The gum edge where it meets the tooth should look clean and pale pink — not red, purple, or swollen. Press gently and release — healthy gums immediately return to pink (this tests capillary refill). If you see anything red or angry-looking, photograph it and show your vet at the next appointment — or schedule one sooner if the redness is pronounced.
What to do: Schedule a vet dental exam within 2 to 4 weeks. Ask about professional cleaning under anaesthesia if tartar is present. Start daily enzymatic toothpaste brushing immediately — Virbac C.E.T. earned its 2026 VOHC seal for both plaque and tartar claims. Consistent home care after professional cleaning is what keeps gingivitis from returning.
Sign #4 — Changed Eating Behaviour ⚠️ Don't Ignore This One
Changed Eating Behaviour — Dropping Food, Chewing One Side, Eating More Slowly
Here is why this sign is #4 and why it is the one we tell every dog owner not to overlook: it is the most commonly misread sign of dental disease in dogs, and by the time it appears, your dog has been in significant pain for weeks.
Think about what it takes for a dog to change their eating behaviour. Their entire evolutionary drive is to eat — wolves and their domestic descendants are motivated by food above almost everything else. When a dog begins dropping kibble from their mouth mid-meal, chewing exclusively on one side of their mouth, eating noticeably more slowly than usual, or showing hesitation before a meal they previously ran to eagerly — they are doing so because the pain has become greater than their instinct to eat normally.
This is not a dog being picky. This is not a dog that "doesn't like their food anymore." This is a dog in genuine, consistent oral pain that has crossed the threshold where even the food-motivation drive cannot override it.

According to VCA Animal Hospitals, signs of dental pain include chewing with obvious discomfort, dropping food from the mouth, swallowing with difficulty, and drooling excessively — sometimes with blood in the saliva. Each of these behaviours has a specific dental cause. Dropping food typically indicates pain when biting down — suggesting an exposed root, cracked tooth, or severe gum inflammation on the side the dog is trying to avoid. Chewing on one side indicates an asymmetric pain source.
Why owners miss this: "He's still eating, so he must be fine." This is the most dangerous assumption in dog dental health. Dogs in significant dental pain continue eating — they are just eating differently. Watch for how your dog eats, not just whether they eat. Even a subtle change in enthusiasm, speed, or chewing pattern is clinically significant at this stage.
What to do: Contact your vet this week — not at the next scheduled wellness visit. Describe the specific change you have observed: dropped food, one-sided chewing, slower eating, blood in drool. Request a dental examination with radiographs. At this stage, X-rays are essential — the Merck Veterinary Manual notes that many dental problems exist below the gum line and cannot be assessed by surface examination alone.
The story behind Sign #4: PetVitalCare founder Sarah M. shared that her dog Max showed this exact sign for six weeks before a vet visit revealed Stage 3 periodontal disease. "He was still eating every meal. I thought he'd just become less enthusiastic about kibble. What was actually happening was that he had two exposed tooth roots causing constant pain." This experience is exactly why this guide exists — and why this sign carries a special warning.
Sign #5 — Pawing at the Mouth or Rubbing the Face
Pawing at the Mouth or Face Rubbing
When a dog repeatedly paws at their mouth or drags their face along carpet, furniture, or the grass, they are trying to physically relieve acute oral discomfort. This behaviour is not a quirk or a habit — it is the canine equivalent of a person rubbing a sore jaw or pressing a hand against an aching tooth. Something in the mouth is causing active, immediate discomfort severe enough to drive repetitive relief-seeking behaviour.
According to Farmington Veterinary Hospital's clinical guidance, face rubbing and mouth pawing are among the most direct behavioural indicators of oral pain in dogs. The Merck Veterinary Manual adds that dogs with dental pain may also show jaw chattering, head shaking, and resistance to having the mouth or head touched — all related pain-response behaviours that owners sometimes attribute to personality quirks or training issues.
Do not confuse normal post-meal face cleaning — rubbing the chin briefly after eating — with the compulsive, repeated rubbing this sign describes. The concerning pattern is pawing or face rubbing that appears multiple times a day without food-related cause, that worsens over time, or that is accompanied by any other sign on this list.

What to do: Call your vet this week. Describe the frequency and pattern of the behaviour. Examine the mouth gently for any visible swelling, redness, or foreign object. If your dog resists having their mouth touched — pulling away, growling, or flinching — tell your vet this specifically, as it confirms the behaviour is pain-related rather than habitual.
Sign #6 — Loose, Missing, or Discoloured Teeth
Loose, Missing, or Discoloured Adult Teeth
Healthy adult dog teeth do not become loose or fall out on their own. If you notice a wobbly tooth in your adult dog, that tooth has lost the bone and ligament support needed to hold it in the jaw — and that loss happened because periodontal bacteria have been destroying the supporting structures, likely for months or years.
According to MedVet's dental specialists, discoloured teeth are equally significant. Healthy teeth should be white or slightly cream — any reddish-brown, purple, or grey discolouration indicates a dead or dying tooth (endodontic disease). The Merck Veterinary Manual confirms that these colour changes signal internal tooth death from injury, fracture, or bacterial invasion of the pulp. A dead tooth that looks "fine" externally can harbour a chronic abscess at the root that never becomes visible until it ruptures through the gum or cheek.
Loose teeth also create an additional risk: attempting to remove a loose dog tooth at home is genuinely dangerous. Dog tooth roots are significantly longer than the visible crown — up to three times the length of what you can see. Incorrect extraction can fracture the root, damage adjacent teeth, or create an entry point for jaw infection. This is strictly a veterinary procedure.
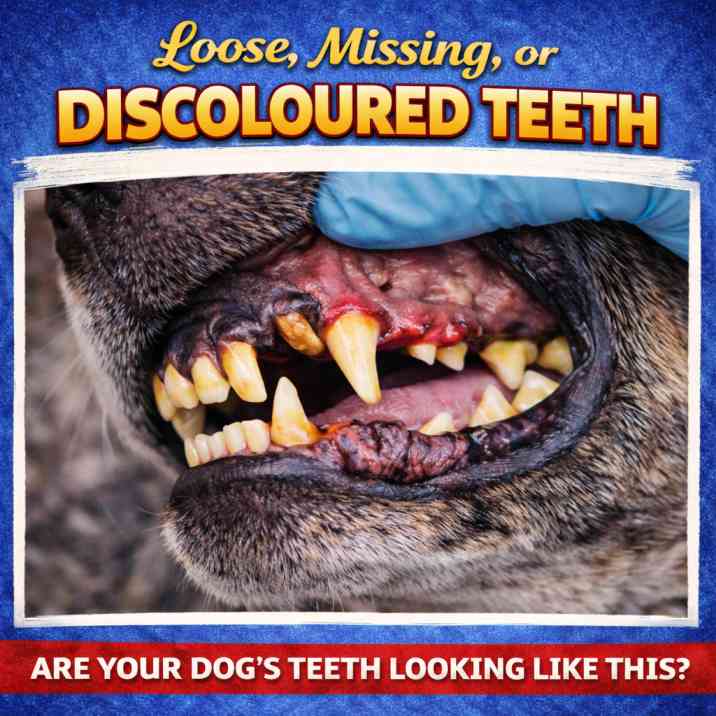
What to do: Schedule a veterinary appointment within 48 hours. Do not attempt to remove loose teeth at home. Ask specifically for dental radiographs at the appointment — discoloured or loose teeth almost always have significant sub-gingival pathology that is only visible on X-ray. At this stage, extraction is typically necessary and is the most humane option to eliminate chronic pain.
Sign #7 — Swelling on the Face, Jaw, or Below the Eye
Facial Swelling or Swelling Below the Eye
A visible swelling below a dog's eye is a dental emergency until proven otherwise. The upper fourth premolar — called the carnassial tooth — is the largest tooth in a dog's mouth and has three roots. Those roots sit directly beneath the bone below the eye socket. When this tooth develops an abscess, the swelling often becomes visible externally as a bump or soft lump beneath the eye.
Facial swelling and swelling along the jaw can also indicate an advanced periodontal abscess — a pocket of infection that has spread from the tooth root into surrounding tissue. As Farmington Veterinary Hospital's clinical team notes, a tooth infection does not stay confined to the mouth. Bacteria can enter the bloodstream and spread to the heart, liver, and kidneys. In the most severe cases, dental abscesses lead to systemic (whole-body) infections that are genuinely life-threatening.
This is also the sign that is most often misidentified by owners as an insect sting, an allergic reaction, or a bump from playing. If swelling near or below the eye appears in a dog that also has bad breath, altered eating behaviour, or any other signs on this list, the dental cause is overwhelmingly likely. Do not wait to see if it goes down on its own.
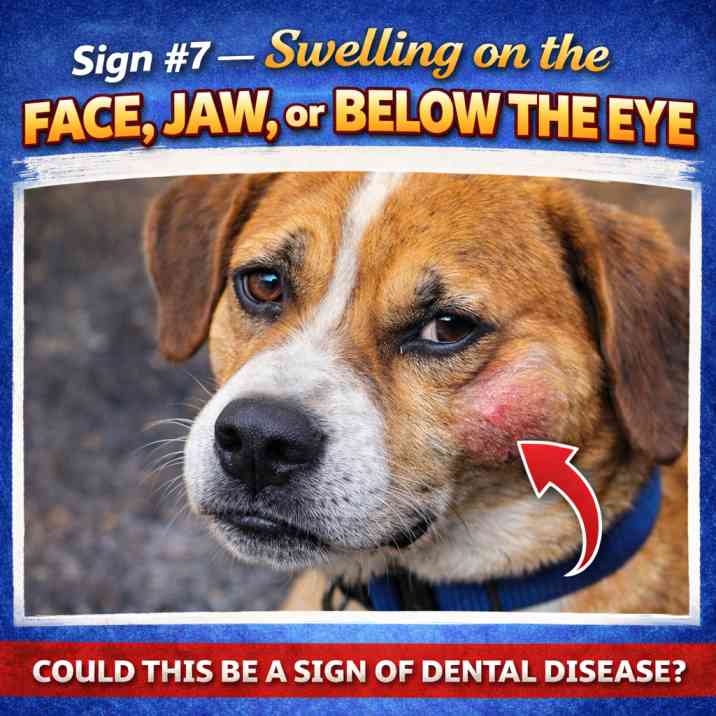
What to do: Call your vet today — same day if possible. If your regular vet cannot see you, contact an emergency veterinary clinic. Describe the swelling's location specifically: below the eye, along the jaw, or inside the mouth. Treatment requires antibiotics and veterinary dental surgery, almost certainly including extraction of the affected tooth. Do not give human pain medications (aspirin, ibuprofen, paracetamol/acetaminophen) to your dog — all of these are toxic to dogs.
The 4 Stages of Dog Dental Disease — Where Is Your Dog?
Dental disease in dogs is classified in four stages by veterinary dentists. Knowing which stage applies to your dog tells you what treatment is necessary, what it will cost, and what is still reversible. The signs above map to these stages as follows:
| Stage | What's Happening | Signs You'll See | Is It Reversible? | US Cost 2026 |
|---|---|---|---|---|
| Stage 1 — Gingivitis | Plaque and early tartar. Gum inflammation. No bone loss yet. | Bad breath · Red gum line · Early tartar visible | ✅ Fully reversible | $100 – $300 |
| Stage 2 — Early Periodontitis | Gum pockets forming. Up to 25% bone loss around some teeth. | Heavier tartar · More pronounced gum redness · Mild eating changes | ⚠️ Partial — can stop progression | $300 – $600 |
| Stage 3 — Moderate Periodontitis | 25 to 50% bone loss. Gum recession visible. Significant bacterial load. | Visible eating pain · Pawing at mouth · Gum pulling away from teeth | ❌ Bone loss permanent — stop further damage | $500 – $1,200 |
| Stage 4 — Advanced Periodontitis | Over 50% bone loss. Loose teeth. Possible abscess. Systemic risk. | Loose teeth · Facial swelling · Severely altered eating · Blood in saliva | ❌ Irreversible — extractions required | $800 – $3,000+ |
The most important fact in this table: Stage 1 is the only stage that is fully reversible. Every stage after it involves permanent loss of supporting tissue or bone that no treatment can restore. The signs in this article — bad breath, early tartar, red gums — are Stage 1 and 2 indicators. Catching and acting on them early is the difference between a $200 cleaning and a $2,000 surgery.
⚠️ When to Call the Vet — Urgency Guide
🚨 Vet Today — Do Not Wait
For UK and European readers: Contact your registered vet directly. If outside business hours, use your vet's emergency line or an out-of-hours emergency clinic. The PDSA PetAid service is available in the UK for owners who qualify. Do not give human pain medications — aspirin, ibuprofen, and paracetamol are all toxic to dogs.
What to Do Tonight — Prevention That Actually Works
If your dog currently shows none of these signs — or only Sign #1 (mild bad breath) — you are in the ideal position to act before disease progresses. This is the routine that prevents dental disease from ever reaching signs #4 through #7.
Daily brushing with enzymatic toothpaste — 60 seconds
The single most effective preventive action available. Focus on the outer surfaces of the upper back teeth — where plaque builds fastest. Use only dog-safe enzymatic toothpaste. Virbac C.E.T. (VOHC seal 2026) and Petsmile Professional (VOHC-approved for plaque inhibition) are our top-tested picks. Even 30 seconds daily beats 2 minutes twice a week.
One VOHC-approved dental chew daily
Give one VOHC-approved dental chew sized for your dog's weight every day. Options with VOHC approval: Greenies Original, Whimzees Naturals, Oravet Dental Hygiene Chews, and Milk-Bone Brushing Chews. Non-VOHC chews have not passed independent clinical trials — their dental claims are marketing, not evidence.
Water additive in the bowl daily
Add a tasteless water additive like Oxyfresh to fresh water every time you refill the bowl. The Oxygene technology neutralises odour-causing bacteria on contact — passively, every time your dog drinks. Ideal supplement for brush-resistant dogs and as an addition to daily brushing for maximum protection.
Annual (or biannual) professional veterinary cleaning
Colorado State University's Veterinary Teaching Hospital and the AAHA both recommend professional cleanings at least annually for adult dogs, starting at age 1 for small breeds and age 2 for large breeds. Small breeds — at highest risk of periodontal disease — often benefit from biannual cleanings. No home care routine substitutes for professional sub-gingival scaling.
Monthly at-home mouth check
Once a month, in good lighting, gently lift your dog's upper lip and check the gum colour, tartar level, and tooth colour on both sides. Look for the warning signs in this article. Takes 30 seconds. Document what you see — a quick phone photo of the teeth every month creates a comparison baseline that helps you spot changes before they become serious.
🛒 Vet-Recommended Products That Work — 2026
Frequently Asked Questions
The earliest observable signs of dental disease in dogs are persistent bad breath — breath that is consistently offensive at normal distance rather than mildly unpleasant up close — and visible yellow or tan discolouration along the gum line of the upper canine and back teeth. At this stage, the disease is still in Stage 1 (gingivitis) and is fully reversible with professional cleaning and daily home care. The challenge is that these signs are subtle enough that many owners normalise them or miss them entirely.
Dropping food during meals is a significant sign of dental pain. Dogs are motivated by food above almost everything — when a dog drops food consistently, the pain from biting down has crossed the threshold where even hunger cannot override it. Common causes include an exposed tooth root, a cracked or fractured tooth, severe gum inflammation, or an advancing periodontal abscess. This symptom warrants a veterinary appointment within days. Request dental X-rays specifically — the cause is almost certainly sub-gingival and will not be visible on surface examination alone.
Yes — and this is the most dangerous aspect of canine dental disease. According to VCA Animal Hospitals, few dogs show obvious signs of dental disease even when the condition is advanced and painful. Dogs evolved as predators and instinctively hide vulnerability and discomfort. A dog may be in significant chronic pain from periodontal disease while continuing to eat, play, and behave normally. This is why the warning signs in this guide matter — and why regular veterinary dental examinations are essential, not optional.
Red gums in dogs indicate gingivitis — active inflammation caused by bacterial toxins in plaque and tartar at the gum line. Healthy gums should be pale pink, firm, and should not bleed when gently touched. Any redness, swelling, or purple discolouration along the gum edge is a sign of active bacterial inflammation. Gingivitis is significant because it is the last fully reversible stage of periodontal disease. Professional cleaning and consistent home care at this stage can return gums to full health. Once gingivitis progresses to periodontitis, tissue and bone damage is permanent.
Costs increase dramatically with disease stage. A Stage 1 professional cleaning costs $100 to $300 at most US veterinary clinics in 2026. Stage 2 to 3 treatment — including deep scaling, dental radiographs, anaesthesia, and possibly extractions — typically costs $500 to $1,200. Advanced Stage 4 disease requiring multiple extractions or jaw surgery can reach $2,000 to $3,000 or more. A complete daily prevention routine (toothpaste, dental chews, water additive) costs approximately $40 to $60 per month — roughly one-quarter of the cost of a single Stage 1 cleaning, spread across the month.
Not always, but in dogs it is a dental problem until proven otherwise. The upper fourth premolar (carnassial tooth) has three roots that sit directly beneath the bone below the eye socket. When this tooth develops an abscess — which is common in dogs with advanced dental disease — the infection often presents as a soft swelling below the eye. This is a dental emergency that requires same-day veterinary attention. Treatment includes antibiotics and typically extraction of the affected tooth. Do not wait to see if it resolves on its own — dental abscesses do not resolve without treatment and can spread to surrounding bone.
The Bottom Line — April 2026
Eighty percent of dogs over age three have dental disease. Most of them are showing at least one of the seven signs in this article right now — and most of their owners have not yet connected what they are seeing to a dental problem.
The signs progress in severity: bad breath and early tartar are your warning to start home care and book a dental check. Red gums are your last chance to reverse the disease completely. Changed eating behaviour — Sign #4 — is your signal that the pain has become too significant to hide. Pawing, loose teeth, discoloured teeth, and facial swelling are emergencies that need a vet this week or today.
Start tonight. Lift your dog's upper lip. Look at their gum line and back teeth. Note what you see. Then use the prevention routine above consistently from this point forward. That single habit change — started tonight — is the thing that prevents Stage 1 from becoming Stage 4.